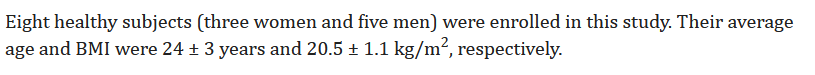Not needed, just eat your proteins.
Maintain on 72 hr fast plus OMAD for 4 days after?
If you already bought the protein powder, use it, fine. But for your muscles and for your body in general you need protein. Meat, eggs and other sources are perfectly fine, the powder has no magical things and as you do keto, you can eat tasty fatty protein  Most bodybuilders do the low-fat approach. Some have boring food ideas only and too often some insanely high protein minimum they can’t do with lean meat… At least the amateur bunch I met online was like that. The smarter, more knowledgeable ones kept educating them…
Most bodybuilders do the low-fat approach. Some have boring food ideas only and too often some insanely high protein minimum they can’t do with lean meat… At least the amateur bunch I met online was like that. The smarter, more knowledgeable ones kept educating them…
I have many medical journal links which say otherwise, here is one for example that I did not post in the other thread https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6312800/ and here is a quote from it.
" In healthy subjects, a high animal protein diet induces hepatic insulin resistance due to glucagon excess compared to a normal protein diet. Nondiabetic subjects on a high protein diet show increased gluconeogenesis and hepatic glucose output compared to subjects on a normal protein diet. Further, the normal suppression of hepatic glucose output by insulin is impaired in the subjects on a high protein diet compared with those consuming a normal protein diet. Glucagon secretion correlates with the magnitude of the impairment, indicating that impaired inhibition of hepatic glucose production by insulin is mediated by enhanced glucagon secretion [80], [98].
In patients with T1D and T2D, the increase in plasma glucagon associated with animal protein intake is accompanied by an increase in plasma glucose despite a constant infusion of insulin, suggesting that animal protein intake contributes to the post-prandial hyperglycemia through an increase in glucagon secretion [29]. Consistently, dietary animal protein increases insulin requirements in patients with T1D. The post-prandial rise in plasma glucose and therefore the insulin requirement for glycemic control is greater after the ingestion of a standard meal with added animal protein than following a standard meal with added fat. The addition of animal protein but not fat energy to a meal intensifies insulin resistance and therefore increases the amount of insulin required for metabolic control. The added protein to the standard meal activates glucagon secretion which in turn amplifies insulin resistance [99]. Similarly to healthy humans, the rate of gluconeogenesis and hepatic glucose output is increased in patients with T1D on a high protein diet compared to a normal protein. Further, the ability of insulin to suppress hepatic glucose output in the high protein group is reduced compared to the normal protein group. A marked parallelism between hepatic glucose production and glucagon secretion is observed, indicating that impaired inhibition of hepatic glucose output by insulin is mediated in part by enhanced glucagon secretion in the patients with high animal protein intake [80]."
Can you please give recent links discrediting the medical journals which repeatedly note that GNG is increased with protein intake absent concurrent carbohydrate consumption?
Interesting issue. I’ve been trying a TKD (targeted keto diet), where you (or I) eat carbs after a workout. For me, I do this only for body weight training workouts, which for me are about 1:10 to 1:20 for my “short” workout and 1:20-1:xx (as high as 1:50) for my “long” workout.
I may also use carbs if I go jogging, then do a lot of physical work around the house. I do this because my body weight workouts are the next day, and I found I could not have a body weight workout if I did not eat some carbs. That is, I had to delay my body weight workout until the next day. I did this several weekends in a row, so one weekend, no carbs = had to delay body weight training; the next weekend, had carbs = did not have to delay body weight training.
If I do not combine extra physical labor with jogging, I find low carb/keto does fine to replace the glycogen (or whatever it is) that I need to jog one day and do body weight training the next.
Back to the issue of “refined carbs”. The last 3 workouts, I’ve used a Japanese sweet potato for my TKD. Why? Because normal sweet potatoes cause me issues. Sadly, I had digestive issues with the Japanese sweet potato. Ugh.
I’d rather find something with more nutrition, but instead what does not cause me issues are these things (rice noodles):
These are also easy to make, and you can weigh them and get whatever level of carbs you want.
What I see pretty much everywhere is one item that does not appear to cause many people digestive issues, if you want to eat carbs, is white rice. I have also tried pre-made rice, but that did seem to cause a few issues. But that might be because it’s pre-made, and I really don’t want to try to get regular rice, as I only need a small amount.
Back to your original question, I personally have a hard time doing OMAD. I’ve been doing this in lieu of fasting 36 hours, because everyone is home now. But only 1 day a week. I workout in the mornings, which mean I can’t make it to dinner for OMAD. Instead, I do 2MAD most days.
I read that paper as far as the sentence, “Multiple prospective investigations demonstrate that the intake of animal protein is associated with increased risk of developing T2D compared to vegetable protein.” This has certainly not been the case with me, since it was cutting carbohydrate intake and any associated vegetable protein that reversed my metabolic condition (I was not yet diagnosed as diabetic but was well on the way). So I would question the validity of the association on which their argument relies. If association in this case really did represent causation, they’d have a better case, but I suspect that looking at the studies on which the authors of this paper are relying (they do not cite them, unfortunately) would reveal the possibility of confounders that have not been taken into account.
The authors’ Table 1 is interesting, but it fails to state what insulin is doing under the listed conditions. Bikman et al. showed that the hormonal response to protein is determined by the metabolic milieu. In cases of high carbohydrate intake, insulin responds to the glucose load by increasing, and glucagon responds by remaining low. The insulin/glucagon ratio thus increases significantly. In cases of sufficiently low carbohydrate intake, insulin and glucagon both respond by increasing, keeping the insulin/glucagon ratio low, and allowing ketogenesis and gluconeogenesis to occur in the liver. The things I’ve read have all suggested that insulin resistance is not caused by glucagon, as the authors of this paper maintain, but rather by a number of other mechanisms that vary by cell type (every cell in the body responds to insulin, but what they do in response varies from organ to organ).
I think that what the authors of this paper are neglecting is the complex interaction between insulin and glucagon. They are both produced in the Islets of Langerhans in the pancreas, and they regulate each other. Furthermore, the amounts of these hormones secreted go directly to the liver first, where they are further regulated before being released into the bloodstream. This is one of the difficulties of insulin treatment for Type I diabetes, because it is impossible to imitate this secretory pathway with a hypodermic injection.
The authors also have some confusing things to say about pancreatectomies that also make me think they haven’t thought things through (though, to be fair, this may be more a problem of translation), since they appear to be talking about insulin resistance in the absence of endogenous insulin production as being a glucagon problem. Whereas it seems more likely to me that insulin resistance in such a circumstance is more likely the result of overdosing than of glucagon production. In mouse models where the pancreas’s ability to produce glucagon as well as insulin has been destroyed, the mice do not develop diabetes, suggesting that there are other regulatory processes that come into play in the absence of insulin and glucagon.
A fair response , but my question stands since I have many links I could throw up. Who has shown your statements and when and where? I was looking for a viable source for a differing opinion, since my searches keep coming up with papers that note the same conclusions. Can you provide some links that high protein intake does not increase GNG since I am confident you should not try to argue with every medical journal publication I read.
Can you provide some links that high protein intake does not increase GNG
I don’t think such studies exist. Not because they couldn’t, but they don’t. No one is studying GNG for protein for people in low carb/keto.
Here’s one, but this uses keto with high protein versus low protein, but high carb:
Can’t find anything where keto people are used and high versus low protein is used.
Forgive me as I’m whatever the opposite of a scientist is, but I’m intrigued by this stuff…is this study on point here?
To be honest, it doesn’t really matter. GNG is meaningless for 99.999% of folks (T1 and maybe T2 excepted). For instance, I’ve tried high fat or high protein many, many times since 1/1/14. I always come back to high protein, as I feel the best and lose the most weight. For me, whether higher GNG is or is not happening is immaterial.
But those people weren’t keto:
So, it’s unclear how their results would apply to keto folk.
And, they were healthy volunteers. While I consider myself fairly “healthy” (to the extent one can even define this), I’m still recovering from decades of high carb, then high carb + high PUFA intake. I may not be like these “healthy” (read: young) volunteers.
Have them gain 25 years, 90+ pounds, lose a lot that, go keto for 8 years, and then take that test.
Edit: By the way, does anyone else think that 20.5 + or - 1.1 kg/m^2 is potentially one of the most useless measurements ever? If someone is 2 meters (about 6 feet) tall, how much do they weigh?
Thanks for post this link. I hate to say this, because the study confirms my preconceptions, but it is low-powered. Eight subjects, only three of them women, means difficulty distinguishing the signal from the noise. And what I could make of the description of their method was intriguing, but I wonder about some of their choices.
Still, I suppose this is one of the studies from which the current lack of concern over protein intake stems.
I didn’t read that far in the study, but on the face of it, I agree with you. 
Two meters, by the by, is six feet, six inches, and someone that tall had better weigh around 210-220 lbs. (95-110 kg) to be healthy. (I’m going by the heights and weights of Boston Bruins players, btw. They are clearly healthy and not carrying much fat.)
Aye, that one is one of my references within the post GNG, protein and blood glucose re-visited and I discuss it briefly. Overall it shows that in the absence of carbs, a smaller but significant portion of the protein (8% if memory serves) is used for glucose production, within a population of SAD eaters for one meal that was not particularly excessive in protein (again if my memory serves correctly). Not quite equivalent to showing excess protein is not converted into glucose.
I have read that for glycogen depleted athletes or fasters the percentage could double to 15%+. Still looking at the word excess as well though, which may not even be well defined.
Part of the confusion on this topic is that many still are stuck on insulin model without the recognition that glucagon promotes GNG independent of insulin since glucagon responds to amino acids much greater than it responds to insulin. Protein stimulates glucagon and GNG while also stimulating insulin and glucose absorption - a strange pairing.
Thanks for that link, one that I have in my link library (read a while ago now). Thought it was going to go into mitochondrial decoupling originally.
According to Bikman, the key is the insulin/glucagon ratio, which in the case of protein eaten on at low-carb diet, stimulates the secretion of both hormones, thus keeping the ratio low.