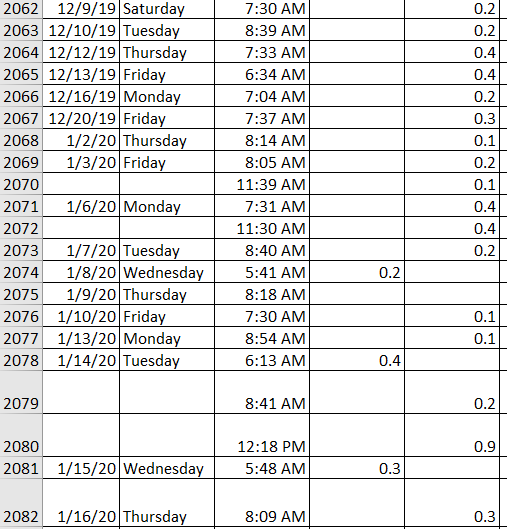What is the immune repair range? Is it the Ketone to Blood Glucose Ratio? Aiming for 1:1 or more toward blood ketones for therapeutic effect.
Paleolithic Ketogenic Diet
Sorry, I didn’t mean you should search that long. If I knew what keywords to use, I’d search too.
I’ve been adding more fat (mainly suet) to my lean-meat lunches to see what effect this has. It might have an effect, but I’ve also restarted 36 hour fasts, though only one per week the last two weeks. Hard to tell what’s more important.
Due to having some issues, I also stopped taking anything other that Mg and vitamin D. This also throws a wrench into the works.
@FrankoBear You’re probably correct about the immune repair range.
I stopped trying to calculate GKI when I realized I had ketones of 0.1-0.2 mmol/l in the morning. I never have a good GKI in the morning, unless I fast multiple days.
Now, if I take this in the evening, I can get a better GKI, but still not great. I just don’t make the ketones I used to.
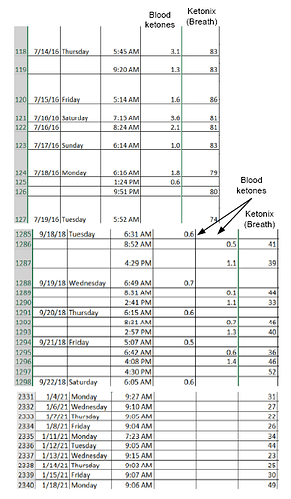
This shows why, though for some reason I skipped the part showing 0.1-0.2 BHB every morning:
I’ll toss some BHB tests in, just for posterity’s sake:
There are two entries, because I had two meters, one for home and one for work.
Still have not located the O’Hearn ref, but here’s something from Phinney/Volek that might help understand how/why ketone concentration varies; but it never actually stops! They mention FFA availability as related to ketone synthesis, although they don’t say the liver pathways must first be at max cap before ketone synthesis ramps up from baseline.
Thanks, Michael. I also found this:
This seems the most plausible part to me:

I have to contemplate that I never stopped exercising and work out 2-3 days a week. If you assume 2x/week, 50 weeks a year, 7.5 years, that’s at least 750 times I’ve exercised. And this doesn’t count all the house projects I’ve done, many of which cause my heart to race (been thinking of wearing a pulse monitor, but can’t remember to do so). And that includes many work outs done after 32 or so hours of fasting.
I hypothesize that my muscles are outstanding at using free fatty acids for fuel, basically short-circuiting my “need” for ketones.
I guess I could get a FFA test, exercise, and get another FFA test to see what happens. But would that test this theory? What if I make FFAs while exercising?
Anyway, I do find, like the Mark’s Daily Apple article says, that I can get higher ketones if I eat higher calories/fat one day. It’s transitory, though.
This is exactly what O’Hearn talks about:
What about people on long term ketogenic diets who still get astronomical readings? What’s going on?
A major factor not often mentioned in whether someone on a keto diet blows high or low ketones is overall calorie intake. How much food are you eating?
Ketones are generated when the amount of dietary fat available to be burned exceeds the supply of oxaloacetate (provided by protein or carbohydrates). It’s not that the body thinks, “This woman needs some ketones, stat.” It’s more like, “I’ve got too much acetyl-COA from all this fat, and I can’t find any oxaloacetate. Guess it’s ketones!” If you’re the type to use keto to justify chugging olive oil, you’ll generate lots of ketones simply because your fat intake is outpacing the supply of oxaloacetate. Keto athletes eating tons of calories will probably produce more ketones simply because they’re eating so much fat.
Questions about Protein
If one wants higher ketone readings don’t they just eat more monosaturated oils and fats?
I used to bomb coconut oil to get a keto high.
I think we previously covered how Omega-6 fatty acids generate higher ketone readings.
Somewhere in the types of fats and oils is the therapeutic GKI masked by a faux high ketones manipulated by inflammation causing oils. But maybe they don’t because they are being metabolised into ketones before being incorporated into body tissues?
@amwassil Thanks for the O’Hearn quotes.
What she doesn’t explain is why this changes over time, although the diet doesn’t change much. If anything, I’m eating higher fat now than I did say a year ago, but my ketone levels are no higher (at least by Ketonix – have Precision Xtra strips added to my cart, but haven’t purchased them).
Now, I don’t have exact numbers (which wouldn’t be “exact” anyway), as I’m not weighing everything, but I am adding more fat to my lean meats to see what happens. Even ate lean beef (cold) with butter the other day.
To @FrankoBear’s point, though, I’m adding mainly MUFAs and still trying to add sat fat while limiting PUFAs. So, suet (mainly MUFA, but “high” in sat fat too), with A2 cheeses at times to up the sat fat, and some sat fat in the evenings (10% fat yogurt, sometimes with cacao butter).
I’m still leaning to the FFA theory and my muscles directly using FFAs instead of ketones. This means that even if I did increase PUFAs, I wouldn’t get the same result in increased ketones now as I did say 3+ years ago. My body has figured out I don’t need the ketones as much.
Unfortunately, all I have right now to test is my ketonix (breath ketone analyzer), which is tough to interpret. Sometimes, it does seem like eating more fat the day before causes a higher reading; other times, not so much. And if calories factor in there, that makes it even harder to interpret, since I’m not counting calories.
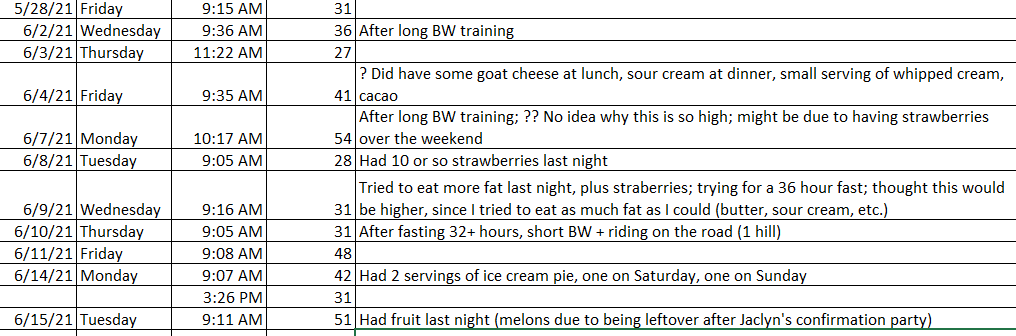
My ketonix readings vary from 21-51 lately, still a far cry from the 70-80+ a few years ago. And as with many of my n=1 tests, the results I thought I would get often don’t show up. See June 9, when I tried to eat high fat the day before (due to wanting to fast, and subsequently doing so). Thought I’d get higher results, but didn’t. Lots of data points here I thought would be different.
This is what Dr. Phinney and others have been saying since before I embarked on a ketogenic diet. I didn’t realise it was in question. Part of adaptative glucose sparing (i.e , physiological insulin resistance) is supposed to be the sparing of not just glucose but also ketone bodies for organs that need them more. It would make sense at that point for the liver to better match production to need, I should think.
Not hers. From the article you linked. Just noting it’s very similar to what she said that I can’t seem to find again.
Which is, of course, what ‘fat adapted’ literally means; ie utilizing FFAs directly for energy. Assuming ketosis, the question is why do some folks continue to measure relatively higher ketones after full adaptation while others measure relatively low? The article Bob originally linked above and specifically the part he quoted addresses the ‘why relatively low?’ and the part I quoted addresses the ‘why relatively high?’
My take, maybe I’m missing something? Again, assuming ketosis, if you’re eating not so much fat, eating higher protein and burning mostly endogenous fat, then your liver is going to have plenty of oxaloacetate to oxidize the fat and make fewer ketones. Conversely, if you’re eating more fat and less protein and endogenous fat your liver is more likely to run out of oxaloacetate and start pumping out ketones.
PS: keep in mind that Phinney and Volek studied mostly competitive endurance athletes who were more likely to be consuming more calories and fat than burning endogenous fat. So, higher ketone levels than those of us who aren’t running or cycling through several thousand calories of fat per day.
One in my family has had a dark skin mole cut off their arm. It was a melanoma. They have been going back for PET scans with radioactive labelled glucose. I found it interesting that this melanoma is a glucose user. After 18 months the PET scan found melanoma cells in their armpit lymph node. The diagnosis now is metastatic malignant melanoma. That means a poor prognosis. The PET scan was full body and no other areas or lumps lit up. So, it’s back to regular monitoring.
In general my extended family think my WoE is crazy. So we don’t mention it. But my mother-in-law and my mum feed me a lot of meat and some green leafy vegetables. There are no pasta, noodles, bread or starchy vegetables. So, I reckon they understand. This presents a conundrum. Because the melanoma is glucose fuelled it would probably be worth considering a therapeutic keto WoE. The cancer patient eats a 3MAD mainly home-cooked wholefood diet, with some breakfast cereal. They love a glass of red wine each evening. I know what I want to say. But we all know what happens when we offer up the keto WoE when not asked about it. And keto is a step before PKD.
New DeLauer video on reasons ketones drop
He puts fat adaptation with muscles using FFA directly as the most important
@FrankoBear I would. When I got my CAC scan, they also saw a small nodule in my lungs. I had a different scan done, and they found two small nodules. I’m in a waiting pattern (another scan in about a year), but I’m thinking I should increase fat and decrease protein (somewhat, anyway), and get back to longer term fasting. Also saw a (mouse) study where they used metformin on fasting days, to further limit the growth of tumors. I might try that.
I just find it interesting that when I started taking my ketones, I was about 1.5 years into low carb/keto, and yet could still get 3.0+mmol/l BHB in the morning with no issues. Didn’t need fasting.
Fast forward a few years and I get 0.1-0.2 mmol/l BHB in the morning, and can’t get above/near 2.0 mmol/l unless I fast 4+ days, and then only in the evening.
Does it really take 4-6 years for this to happen? Am I an outlier? Or is this normal?
Unfortunately, I know very few people who have had the same length of time as I’ve had for keto/low carb, and who also exercise at around the rate I do (about 3-4 hours per week), using the exercises I do (short HIIT workouts either alone or with body weight training to failure, and a long body weight training to failure 1x/week).
I have found that adding beef suet to my lean meats (beef heart today) does seem to give me more energy. Ms. O’Hearn could be correct. Which might make Ted Naiman and Mr. Kendall wrong, at least for me.
Still testing, though.
I have been doing Keto for 1.25 years. My ketones at 11AM (fasted) were 0.3 mmol today. That is after a period of prioritizing fat including yesterday. By consuming fat (usually HWC in my coffee, recently MCT oil and sometimes coconut oil) I can get that up to say 0.7 maybe 1.2 if I lean on MCT oil. I have even tried exogenous ketones and have gotten to 2.2. I think that is the max i have seen.
Today I am just going to keep fasting to see what happens. I also do a lot of exercise.
My intuition would be that not so much should change between 1.25 years on keto and 7.5 years on keto. I would hope it doesn’t take our bodies that long to optimize a new fuel source (talk about a new level of metabolic inflexibility!) - but we are all probably highly individual.
I’ve already had cancer and wish I had known about keto back in 2008.
Would definitely adjust my diet if it came back - from keto to therapeutic keto.
I think you hit it here: “but we are all probably highly individual”. Each of us has a very different and unique history of metabolic abuse and damage caused by years/decades eating high carb and industrial seed oil PUFAs. Maybe ethanol, too. What specifically got damaged, how extensive and severe the damage and even our genetic resilience determine how long it takes to recover metabolic health. Some will recover full metabolic health relatively quickly and easily and some may never recover fully. So, yes, metabolic inflexibility may be chronic for some. What’s on your plate does not make metabolic flexibility. What your cells do with it does.
Is the difference just the increased fat and keeping BHB levels high (with glucose low)? Or is it more complicated?