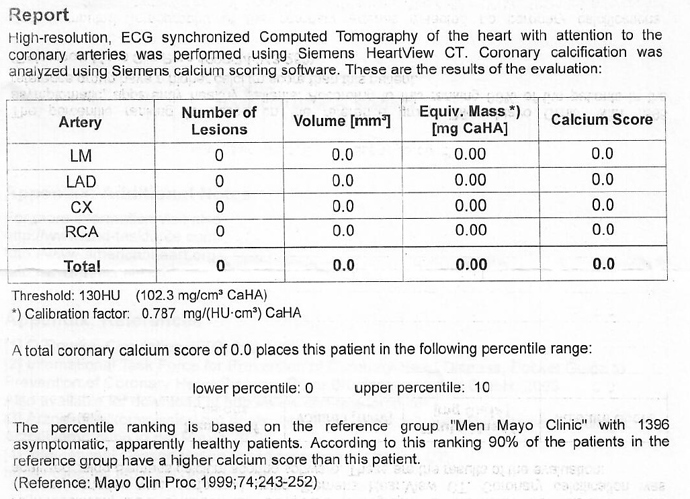
No, a lot of places provide a sort of estimate of five- or ten-year risk of a cardiovascular event along with the actual score.
My sharply rising CAC score - and why I'm staying the keto course 🖖
Oh, I know what you’re referring to. No, I don’t see that sort of info included in the results provided.
I guess I’ll now share an interesting side story I refrained from raising as it might just add to potential confusion…
BACKGROUND: My wife and I get our CAC scans together each year same time/place. Each test, along with mine, her scores have also risen since we’ve been keto - although, in candor, she is not as 100% consistent as I am in avoiding non-extraneous carbs (i.e., from time to time she might indulge in some rice or perhaps fruit, which I don’t). Still, I do our cooking and she’s generally pretty keto-adherent.
WEIRDNESS: While her scores have also been rising (to 240 from 163 prior year) the strange thing in her case is that her components moved in sharply opposite directions, as follows:
LEFT ANTERIOR DESCENDING: rose from 103 to 239
LEFT MAIN ARTERY fell from 60 to ZERO.
In other words, the same blood circulating through the same heart made ONE artery double in its calcium score while it made the ANOTHER artery clear up from 60 to no measurable calcification at all.
This makes me wonder how such a thing could be - and more importantly, what it means. 
I don’t know. Whenever we base something on so few samples, I get concerned. Now, they used this in the so-called gold standard hyperinsulinemic–euglycemic clamps, but I’m not those people. I’ve been eating a low carb diet for over 7 years. I have high “insulin resistance” every morning, and have had it for years:
Is what’s measured on less than 5,000 people, who did not eat what I eat and have not been on the diet I’ve been on for as long as I’ve been on it, applicable to me?
And that score appears to only be used for “insulin resistance” and a tend toward diabetes, and not heart disease. In your and my case, you get a much better LPIR score, but your CAC is 207, whereas mine is zero.
What does this mean? Does this mean a lower LPIR score means worse CAC? I don’t think so, but the score seems to be misleading, at least our (potentially outlier) cases.
Beats me 
If the cohort were relevant and the research were well-constructed, I’d have no problem with 5000 (assuming the sample variances were significant enough to produce statistical significance). Absent this, I wouldn’t rely on a study of 500,000 (e.g., if all were eating SAD-style and found that too much saturated fat became problematic) since - to your point - it would be unreliable/irrelevant to our situation.
But I (heartily) agree that our conflicting test results are a bit of a puzzle. Given a choice, I’m not sure which profile I’d rather have. Probably a good thing we don’t get to choose - I’d likely pick wrong.
There are numerous things beyond diet and cholesterol that have associations with CVD such as heavy metals poisoning, mold toxins, bacterial infections, etc. Although I’d expect most such things to have some sort of symptoms if they are bad enough to accelerate CVD. Since you are feeling great your approach seems reasonable to me. I’d likely repeat the CAC scan in a few years. If your speculation is right I’d expect to see stabilization or a slowing rate of growth in score.
Good counsel. I do plan to repeat the CT scans at some point in the future and will share the results here accordingly. Meanwhile, I will be staying on the keto path (if inflammation is underway, got any better alternatives?)
I was never a fan of heavy metal, and so I shall stick to jazz, classical, and perhaps some early rock. 


@ctviggen Just another thought on your CAC score of zero…
As you know, you’re not unique around here. There are a significant number of (older) males with zero CAC scores on this forum - i.e., no measurable calcification.
Yet, by the age of 55, more than 60% of men in the general population have some detectable (non-zero) coronary calcium as measured by CT scan. And by the time men reach 64, less than 20% have a non-zero CAC score.
Appreciating that correlation does not prove causation, we also know that a lack of correlation suggests absence of causation, which would suggest that keto is not causing calcification.
If keto produced calcification, the incidence of older men with non-zero CAC scores around this forum would likely be much higher than it appears to be.
[DISCLAIMER: Obviously this conclusion is for entertainment only, being entirely UN-scientific in every respect. But amuse me further…]
Those of us reporting non-zero CAC scores on this keto forum were shocked and disappointed (like me!) - since we assumed keto would “protect us” from calcification. Of course, we don’t know how much calcification was caused by SAD-style eating for all those decades beforehand.
My own situation is that I’ve gone from a non-zero score (measured around the time I embarked on keto) to an even higher non-zero score, to yet another higher non-zero score over the course of 2 years - all the while diligently keeping my net carbs to around 25g/day.
Yet, also during this time, the low-level body-wide inflammation I’d been experiencing pre-keto has clearly dissipated. It’s reasonable to assume that any arterial soft plaque production due to systemic inflammation should now be easing too - if not stopped completely.
While I certainly don’t like the direction my CAC scores are going, I take solace in the fact that so many others around here eat LCHF and continue to have a zero CAC scores.
And so it further supports (the hope) that my calcification likely reflects whatever my body needs to do to repair whatever soft plaque damage I never knew I had prior in life.
Of course, if this doesn’t make directional sense to anyone with greater knowledge and insight, I’ll gladly invite a correction. 
You just reminded me of something David Diamond says in one of his lectures, to the effect that he and Uffe Ravnskov belief that arterial damage is occurring all the time, and that it is not a problem, so long as the body’s repair mechanisms can keep up. The calcification of soft plaques is part of that repair process, so perhaps what you are experiencing is your body catching up with older damage. It will be interesting to see if the calcification eventually slows and perhaps even reverses itself.
This is what I’m (sort of) hoping is the case. But this idea also has a dark side…
What would this paradigm imply for those with stable CAC scores? … or those with zero detectable calcification?
Does it imply that those without calcification are failing to repair their arterial damage, i.e., the kind that Diamond and Ravnskov suggest is occurring all the time?
If so, not a very encouraging thought for those without calcified plaques 
As any hemophiliac knows, the lack of scabs doesn’t prove the absence of bleeding.
On a more amusing note, this reminds me of something I was told as a kid (which is probably not true, but still makes me laugh):
Female mosquitoes are the ones that bite. Males don’t.
Female mosquitoes don’t buzz. Males do.
If you’re lying in bed and hear a mosquito buzzing nearby, don’t worry.
If you don’t hear a mosquito, it’s time to worry. 
No, it could also imply that damage is being healed short of the need for calcification. In the absence of a real understanding of how the damage occurs in the first place, it is hard to come up with a mechanism for repair.
Diamond and Ravnskov suggest that the vasa vasorum are involved (those being the blood vessels that supply oxygen and nutrients to the coronary arteries), because of where the LDL particles end up in the walls of the arteries. But the standard explanation is that the LDL comes from the blood circulating through the arteries and somehow, through some unspecified mechanism, burrows down through the inner layers of the arterial walls to the outer layer.
Have you tracked your CRP levels to see if inflammation levels have dropped. Considering how you feel, I would anticipate a steady drop in CRP?
Excellent question. Short answer: No, I haven’t.
In fact, I’ve been doing some legwork on CRP-hs - the high sensitivity version of a CRP blood test - intended to get specifically at heart-related inflammation markers.
I haven’t reached a conclusion yet as to whether it’s worth bothering (minimal cost) since any indication of inflammation would be simply suggest I need to eliminate the (inflammatory) carbs … which I’m already doing consistently for two years now.
But since you ask, I wonder whether you have thoughts and/or sources of research info as to how CRP blood levels can inform action plans if inflammation is indeed found?
On the other hand, if a CRP-hs test result shows minimal inflammation, this would provide me further confidence that the course I’m on is the right one? 
Sorry your scores are headed in the wrong direction.
My husband freaked out when one of his arteries came back at 114 (the other two were zero). He was anxious and depressed and angry until he saw our PCP and he said it was nothing to worry about. BUT, if his number increases next year he will be in the same boat as you - wondering what else he can do to stop the progression. His PCP asked if he wanted a referral to a cardiologist (even though he didn’t think it was necessary) and hubby said no.
Been there. Done that. 
Thanks for the sympathy. Given how consistent I’ve been in eliminating carbs, I have a feeling this is actually good news of a sort. Now see if you can convince your husband and let me know. 
We just got ours done a couple of months ago so will be at least 10 months before we get them done again. Mine was zero and my cholesterol numbers have always been worse than his - SAD diet, keto diet.
We’ve been keto for 3 years now - he not as strict as me because his metabolism isn’t trashed like mine.
If it makes you feel any better, the technician giving us our scores saw how upset my husband was and said she’s seen scores over 1000.
Ah, yes, I’ve heard of many folks with 4-digit scores. My “personal best” still falls far short.
Our technician at the hospital wouldn’t offer a clue - she said the cardiologist reads the results and she couldn’t comment. Perhaps she took a glimpse and didn’t want to risk tears. 
Are you going too hard at your HIIT training?
Have you tried direct contact with Ivor Cummins for advice?
I wonder if CAC scores rising would be a worldwide phenomenon during the increased stress of the pandemic.
Two potential paths.
Carnivore eating is an option to test in the low carb eating spectrum in case plant factors are affecting your mineral interactions.
The PaleoKetogenicDiet may be worth researching in its effects on cardiovascular calcification.
I might look at getting my CAC repeated after a year of eating the pandemic. Previous two were 0 and 1.
Other markers of inflammation are white blood cell count (WBC), ferritin, erythrocyte sedimentation rate (ESR), and plasma viscosity (PV). All these readings should be taken into account.
Same pace for 1yr+; not always fun, but feels good afterwards/no soreness.
My confidence in his sound judgment has plummeted as of late.
This has been a totally non-stress pandemic for our family. Wish it were true of most other folks so I wouldn’t feel so guilty about it.
Interesting thoughts … not feeling like those nightly green leafy salads that go with my butter-drenched steak are causing anything, but perhaps you’re on to something here. 
If I had a 0 and a 1, I’d chalk it up to rounding error and quit while I’m ahead.
Thanks for your thoughtful reply.