Your explanation of the preload makes better sense.
Study regarding stevia and insulin release
I keep reading that artificial sugars are 200 X sweeter than sucrose. Nothing tastes sweeter than sucrose to me, not even fructose. Stevia is a bitter herb, barely sweet at all. It is marketed like a health good. I believe sucrose is better for me than stevia. Stevia is nothing more than sales’ hype.
I am pretty sure they dilute them because otherwise it would be a complete nightmare to deal with.
And it honestly depends - if stevia does not cause you to binge, or increase your hunger or cravings then I would disagree. It can be a useful tool.
However, sucrose, if you have insulin resistance is not the better choice in any circumstance imo. If you don’t like the idea of replacements then perhaps it is better to not use either? Sugar is not going to be “good” for people with insulin resistance, period. It is what caused the problem in the first place and is very easy for many to get addicted.
AUC stands for area under the curve. It means they are looking at the total amount of glucose (or insulin, whatever) during a given time period (say 2 hours) rather than just an endpoint or snapshot. If you mentally shade in the area between the glucose line and the x-axis for each substance you can roughly see the area. Otherwise, you need some calculus to get a number value.
No. The point of [both] studies was to see if people would naturally eat more food in reaction to a non-caloric sweetener preload, so the feeding was ad libitum (buffet).
From the 2016 test:
RESULTS: Ad libitum lunch intake was significantly higher for the NNS treatments compared to sucrose
(P = 0.010). The energy “saved” from replacing sucrose with NNS was fully compensated for at
subsequent meals, hence no difference in total daily energy intake was found between the treatments. http://www.nature.com/ijo/journal/vaop/ncurrent/abs/ijo2016225a.html
From the 2010 test:
participants consumed significantly less food over the entire day (including preloads) in the stevia and aspartame conditions compared to the sucrose condition (mean difference between sucrose and stevia condition = 300 kcal, p < .001; aspartame condition = 334 kcal, p < .001). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2900484/
So the tests disagree on whether or not food intake increases.
Forgot the GLP…
GLP-1 is a signalling hormone (incretin) released by the stomach after consuming food. It affects insulin response, among other things. https://en.wikipedia.org/wiki/Liraglutide#Type_2_diabetes
The way I read this is that the sucrose peaks the blood sugar at around 30 minutes, at which point, the insulin response catches up. This is indicated by the down-slope on blood sugar up to the point of the meal. Whatever was in the meal, then, starts to cause a rise in blood-sugar again, but since there’s still left-over insulin, it keeps the blood sugars from rising as high.
The other sweeteners aren’t inducing a large insulin response prior to the meal, so there’s no insulin to handle the carbohydrates in the meal until 30 minutes PP.
Stevia can be processed in different ways. I’ve had some with bitter aftertaste, and some which have no bitterness at all.
I think sylvia may have been a troll of sorts. She posted all her comments on the day she joined, then never posted again.
On the other hand, anyone who thinks sugar has nothing to do with diabetes wouldn’t last long on here, anyway, so…
All I know is that stevia is the least triggering for me and tastes alright among stronger flavors like coffee, cocoa, etc. Conversely, diet sodas make me crave sugar. I guess we’re all different, surprise, surprise.
I have found some illuminating studies on Stevia. I have sensitivities to ALL non-nutritive and artificial sweeteners. I really didn’t want it to be true, so I did a lot of testing on my homemade Stevia extract (bought whole dried leaves and crushed and made my own water extract so it would be totally pure and unprocessed.)
Sadly, I think this explains my experience, and the fact that it is producing an effect I don’t want to perpetuate.
Thoughts?
I suppose if one has chronic elevated insulin heavy stevia use might aggravate the issues of hyperinsulinemia. But the studies you posted are mostly about the positive effects of stevia improving a variety of aspects of glucose metabolism and discussing the therapeutic potential.
I’m a little concerned about researchers’ deriving definite conclusions from associations with high p-values in underpowered studies with few participants. For a discussion of what the interpretative challenges are in such studies, read http://rsos.royalsocietypublishing.org/content/1/3/140216, David Colquhoun’s article on how to interpret p-values. For instance, an association with p < 0.05 is likely to be wrong about 30% of the time.
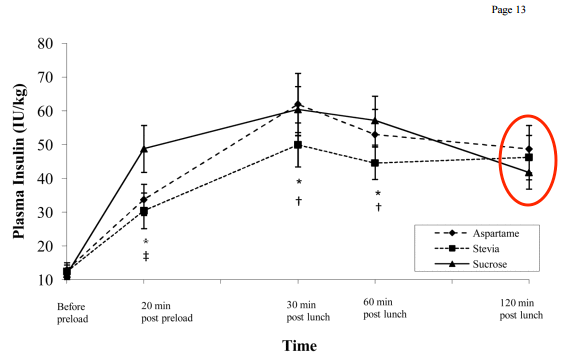
This is a poorly conducted study and it seems like the writers had a strong bias and possibly massaged the data parameters to make it appear in their favor. With regards to keto, the plasma insulin graph is the most important part of this study.
The authors highlight the fact that within 120 minutes, insulin levels were elevated more by aspertame and sucrose than by stevia, and this is true. What they completely leave out, and what is possibly more important, is what insulin levels look like beyond that window. Looking at the graph they published, you can see that at the 2-hour mark, insulin levels are actually higher in the stevia group than the sucrose group. If insulin continues to stay higher in the stevia group than the sucrose group for a significant amount of time, the net result is worse for ketosis as well as for your appetite (you’ll be hungrier).
Without changing the data parameters to extend that window to the point where insulin returns back to normal, this data is incomplete and may very likely lead to incorrect conclusions.
Finally, there is also no control (i.e. no sweetener) in this study, so we can’t even determine from it, whether stevia increases insulin response compared to unsweetened food.
I joined just so I could comment
I am type 2 diabetic Ketogenic for four years.
It was mentioned that the sucrose glucose levels were less at two hours than Stevia.
Excellent point but a mute one when it comes to diabetic glucose response.
For NON DIABETICS it is the insulin response that would weigh most.
The two go hand in hand but the body can deal with higher glucose much better than it does high insulin.
These participants spiked huge from the sugar compared to the others.
Starting at around 80 and finishing at 122 or so but 20 minutes.
That’s a huge increase. 40+ points
It is the spike level that should be considered most when you measure overall glucose responses concerning diabetes.
Yes, high glucose is problematic BUT it is the spikes that do the most damage.
The graph above shows that all levels were around 95 or so at two hours.
And then they cut it off.
The problem there is the glucose levels of Stevia had increased.
A two and a half hour and third hour test would have shown if that upward trend with Stevia was continued OR if it was simply a return to ‘normal’ physiological regulation of glucose.
I find an odd vanilla aftertaste instead of bitter with every Stevia product I’ve tried and it totally ruins my willingness to try the stuff. Lol
So
It is the opinion of this uneducated diabetic that Stevia is definitely a better choice for diabetics.
As for the person saying sugar doesn’t cause diabetes
Right and wrong.
Many things cause diabetes.
Genetics, carbs, lazy butt lifestyles, medications, environmental toxins
Too many suspects to always nail it down to a specific guilty dog
But saying it doesn’t is foolish
But some folks still believe the Earth is flat and that pigs fly on satin wings too.
That is why you seldom see a slim person drinking a diet soda. While the blood sugar may not be there, the sweetness is. This signals the pancreas to pump out loads and loads of insulin. Insulin is a fat storage hormone. This excess insulin causes insulin resistance similar to a person getting drunk on one can of beer. As one continues to drink he/she builds up resistance to alcohol and it takes more and more to get the same buz.
Each cell has insulin receptors. As the insulin settles on these receptors, a signal is sent to open up for sugar. After being bombarded with insulin, over time, these receptors no longer send the signal for the cell to open. So, any sugar in the blood is put into storage around your waist by insulin. I have to go. But, you can reach me at archielloydtucker@gmail.com
I found it interesting that one of the studies cited mentioned that rebaudioside A potentially stimulates insulin secretion at the beta cells. It does not mention reb D. From the limited time I’ve researched various Stevia products, the cheap ones seem to use the bitter (but more available) reb A extract, whereas, the more expensive ones use the less bitter (less available) reb D extract of Stevia. Since the study did not mention reb D, this is merely a speculation and inference, but “you get what you pay for” may make sense in this case. For example, for sweetening beverages I use Splenda Naturals packets (it’s not sucralose based like original Splenda but is only Erythritol & reb D Stevia). They are pricier than others but taste less better to me and concerning the subject of this thread, it may be less insulinagenic as well 
I hope someone weighs in on reb a vs reb d… guess I am off to do some research.
Gut taste receptor research has led to questions on low calorie sweeteners in glycemic control. Effects have been hypothesized based mostly on cellular and/or short-term animal studies. Reported is a 12-week clinical trial investigating the effects of sucralose on glycemic control. Sucralose had no effect on fasting or post-prandial glucose, insulin and C-peptide, or HbA1c.
V. Lee Grotz, et. al, Regulatory Toxicology and Pharmacology Volume 88, August 2017, Pages 22–33
