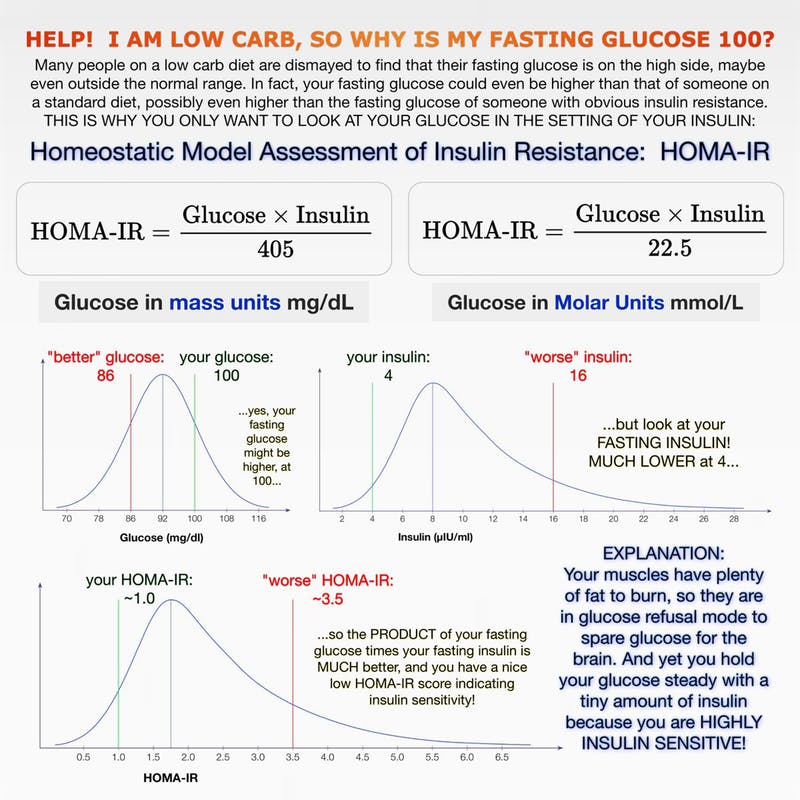
Here is the problem; you want to have a little minor spike in insulin from natural unfreed fructose (when encased in its natural form, such as in fruit and vegetables) that occurs in nature to tell your liver to not go into a constant state of gluconeogenesis because you want to increase your HOMA-IR insulin sensitivity not kill it off completely with a constant steady supply of glucose hence chronically elevated levels of insulin?
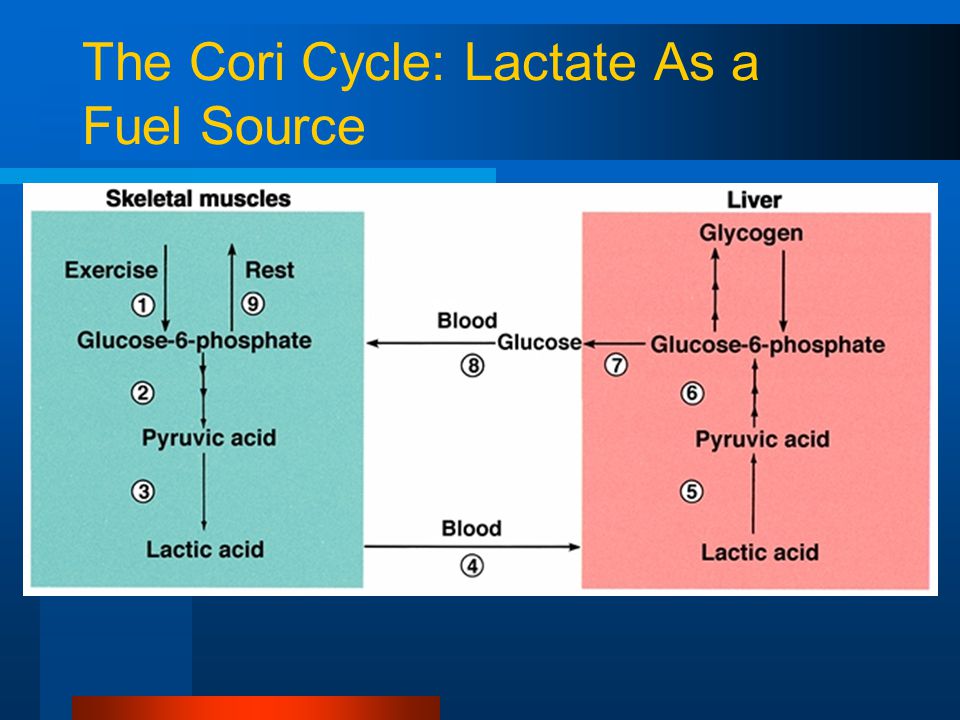
In other words excessive protein will constantly spike insulin however minor but constant and steady and eating natural sugars turns off or inhibits the gluconeogenesis via minor insulin secretions. And yes you still remain in ketosis! If your body needs glucose it is going to pull it from your glycogen storage, glycerol from fatty acids or lactate through the cori cycle so why would you want to supply it with the additional gluconeogenesis?
References:
[1] “…The scientific name is “physiologic insulin resistance” and it’s a good thing — unlike “pathologic insulin resistance.” As regular visitors will know from Dr. Jason Fung, Dr. Ted Naiman, and Ivor Cummins, the “pathologic” kind of insulin resistance is caused by higher and higher levels of insulin — hyperinsulinemia — trying to force glucose into over-stuffed cells. That insulin resistance is a prominent feature of type 2 diabetes, polycystic ovarian syndrome (PCOS) and other chronic conditions. So let’s call physiologic insulin resistance instead “adaptive glucose sparing,” a name that has been proposed by many to reduce the confusion. Dr. Ted Naiman describes it as muscles that are in “glucose refusal mode.” Prior to converting to the ketogenic diet, your muscles were the major sites to soak up and use glucose in the blood for energy. On the long-term keto diet, however, they now prefer fat as fuel. So the muscles are resisting the action of insulin to bring sugar into cells for energy, saying, in essence: “We don’t want or need your sugar anymore, so move it along.” Hence, the slightly elevated, but generally stable, glucose circulating in the blood. Where is that glucose coming from when you consume no sugar and only leafy veggie carbs in your diet? Your liver, through gluconeogenesis — the creation of glucose from non-carbohydrate sources such as lactate, glycerol, and glucogenic amino acids from proteins. It is a natural protective process that got homo sapiens through hundreds of thousands of years of feasts and famines. “There is no essential requirement for dietary carbohydrate because humans possess a robust capacity to adapt to low-carbohydrate availability,” says Dr. Jeff Volek. In the liver of a keto-adapted person, he notes: “ketone production increases dramatically to displace glucose as the brain’s primary energy source, while fatty acids supply the majority of energy for skeletal muscle. Glucose production from non-carbohydrate sources via gluconeogenesis supplies carbons for the few cells dependent on glycolysis [using sugar for energy.]” …” …More
[2] Insulin Resistance is Good?
[3] “…When the body once again enters the absorptive state after fasting, fats and proteins are digested and used to replenish fat and protein stores, whereas glucose is processed and used first to replenish the glycogen stores in the peripheral tissues, then in the liver. If the fast is not broken and starvation begins to set in, during the initial days, glucose produced from gluconeogenesis is still used by the brain and organs. After a few days, however, ketone bodies are created from fats and serve as the preferential fuel source for the heart and other organs, so that the brain can still use glucose. Once these stores are depleted, proteins will be catabolized first from the organs with fast turnover, such as the intestinal lining. Muscle will be spared to prevent the wasting of muscle tissue; however, these proteins will be used if alternative stores are not available. …More
[4] “…The major site of gluconeogenesis is the liver, with a small amount also taking place in the kidney. Little gluconeogenesis takes place in the brain, skeletal muscle, or heart muscle. Rather, gluconeogenesis in the liver and kidney helps to maintain the glucose level in the blood so that brain and muscle can extract sufficient glucose from it to meet their metabolic demands. Go to: 16.3.1. Gluconeogenesis Is Not a Reversal of Glycolysis: In glycolysis, glucose is converted into pyruvate; in gluconeogenesis, pyruvate is converted into glucose. However, gluconeogenesis is not a reversal of glycolysis. Several reactions must differ because the equilibrium of glycolysis lies far on the side of pyruvate formation. The actual Δ G for the formation of pyruvate from glucose is about -20 kcal mol-1 (-84 kJ mol-1) under typical cellular conditions. Most of the decrease in free energy in glycolysis takes place in the three essentially irreversible steps catalyzed by hexokinase, phosphofructokinase, and pyruvate kinase. …” …More