A little recap on what I wrote before in other posts with a few annotations:
If our ingenious peeps down at NIH develop a vaccine (mRNA-1273) fast enough you may not have to worry about it because you will be immune to it in addition to the ketogenic diet protecting your immune system and lungs that you will be able to eat the virus for dinner.
I mean they were feeding the ketogenically fat adapted mice lethal doses of viruses through their nose and they were bulletproof proof against it. Thus Gamma Delta (γδ) in the lower mucosal barrier of the lower lung sacks provide a protective barrier between the host and virus?
Just feeding the mice ketones did no good they just died, it was the fact they were ketogenically fat adapted over a period of time
Being ketogenically fat adapted is supposed to improve immune (anti-bodies ect.) function but how?
I’m sitting here wondering if the thymus gland gets bigger because of ketogenic fat adaption as result of lowered testosterone[6], that’s where T-cells are matured after leaving the bone marrow[1].
If I’m correct then a person who is fat adapted irregardless of age would have the thymus gland of a 12 (annotated) year old (or maybe even a baby?) if testosterone is lowered or blocked from something like fasting or calorie restriction[6]?
Footnotes:
[1] “…Lymphoid progenitors which have developed from hematopoietic stem cells in the bone marrow migrate to the thymus to complete their antigen-independent maturation into functional T cells. In the thymus, T cells develop their specific T cell markers, including TCR, CD3, CD4 or CD8, and CD2. …” …More
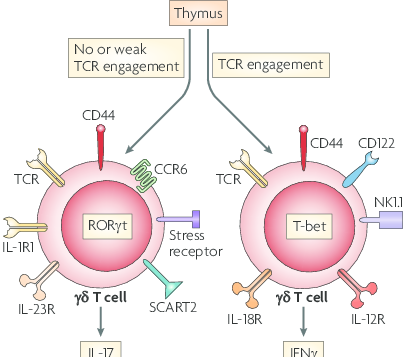 image link
image link
[2] “…A Monash University researcher has discovered how to rewind the body’s immune system back to its youth and re-educate it. Their technique actually re-grows the Thymus gland - the human organ that produces a vital part of the immune system called ‘T Cells’ - so our bodies can prevent and fight off disease. In children, the thymus is about the size of an orange. But once our immune system is set up properly around puberty, the Thymus shuts down and shrinks to the size of a pea. The Melbourne team has discovered how to stimulate the Thymus gland so it grows back to full size and starts producing T-Cells again. They’ve proved it works in mice, and now trials are underway in cancer patients undergoing bone marrow patients. …” …More
[3] “…The sex hormones that flood the body at puberty actually cause the thymus to shrink, which gave Richard his great idea. If he could block these hormones he should be able to get the thymus to grow back and again start pumping out the large number of T cells it once did. …” …More
[4] “…A testosterone-blocker is injected under his skin. The drug will stay in his system for several months and hopefully allow his thymus to grow and produce more T cells so he can get through his low immunity period. …” …More
[5] “…How I Increased My Testosterone by 290% without hormone therapy or sport supplementation. …” …More
[6] ”…Calorie restriction lowers testosterone, except during healthy weight loss. …” …More
[7] Putting mice on a keto diet: Our immune responses to infections are influenced by several extrinsic factors, including weather, social interactions, and diet. Here, Goldberg et al. report that feeding mice a high-fat, low-carbohydrate ketogenic diet confers protection in the context of lethal influenza infection. By characterizing the immune response in the lungs, the authors identified that ketogenic diet promoted the expansion of γδ T cells in the lung. Using mice lacking γδ T cells, the authors have established the functional importance of these cells in conferring protection. Their findings suggest that γδ T cells improve barrier function in the lungs by modifying differentiation and function of the airway epithelial cells. Abstract: Influenza A virus (IAV) infection–associated morbidity and mortality are a key global health care concern, necessitating the identification of new therapies capable of reducing the severity of IAV infections. In this study, we show that the consumption of a low-carbohydrate, high-fat ketogenic diet (KD) protects mice from lethal IAV infection and disease. KD feeding resulted in an expansion of γδ T cells in the lung that improved barrier functions, thereby enhancing antiviral resistance. Expansion of these protective γδ T cells required metabolic adaptation to a ketogenic diet because neither feeding mice a high-fat, high-carbohydrate diet nor providing chemical ketone body substrate that bypasses hepatic ketogenesis protected against infection. Therefore, KD-mediated immune-metabolic integration represents a viable avenue toward preventing or alleviating influenza disease. …” …More
image link
[8]”…It has a clever disguise: Sugars dot the outside of the spike, just like sugars dot the outside of regular human cells, said David Veesler, a structural virologist at the University of Washington who led a team that visualized the SARS-CoV-2 spike and published a March 19 paper on its architecture. This carbohydrate camouflage makes the virus more difficult for the human immune system to recognize. …More
[9] “…There’s also quinine in Tonic Water, which is available just about anywhere at any grocery or liquor…” …More
[10] “…The modern drug is a synthetic form of quinine, which is found in the bark of the Cinchona plant. The plant was taken as an herbal remedy by indigenous Peruvians four centuries ago…” …More
[11] Chloroquine and Quinine are different drugs, the former is now the drug of choice to treat malaria and Quinine, used since 1820, is still used to treat patients with Chloroquine-resistant falciparum malaria. Chloroquine is inexpensive and widely available, used since 1945 to treat a wide variety of illness such as malaria, amoebiasis, HIV, and autoimmune diseases without significant detrimental side effects…” …More
[12] “…Plasmodium falciparum chloroquine resistance is a major cause of worldwide increases in malaria mortality and morbidity. …Chloroquine resistance (CQR) was first reported in Southeast Asia and South America and has now spread to the vast majority of malaria -endemic countries…” …More
[13] “…Areas: Chloroquine - resistant P. falciparum first developed independently in three to four areas in Southeast Asia, Oceania, and South America in the late 1950s and early 1960s. Since then, chloroquine resistance has spread to nearly all areas of the world where falciparum malaria is transmitted. …” …More
[14] Kaiser Permanente launches first coronavirus vaccine trial
*Thymus, the Missing Link in Viral Protection