I’ve been on the KETO & IF wagon going on 4 years and even converted my doctor. I’m well read on the subjects and own, studied and applied about every book printed on the subjects.
That said, I too have seen the physiological/adaptive glucose sparing creature coming into play the past 6 months. My normal fasting G range can be anywhere from 75 to 110 depending on basically my cheat level on carbs but ketone readings always stay in the .5-2.5 rangs, again depending on my activity level and energy intake.
My next physical (Jan or Feb '22)I plan on getting the HOMA-IR score to verify my insulin levels are in fact low as I expect they will be and ratio is good, just for my own peace of mind.
That said, suppose everything checks out and my HOMA-IR and fasting insulin levels are in fact low and I just am seeing the adaptive glucose sparing phenomenon playing out…is or could the excess blood sugar possibly causing harm?
My firm conviction is that the issue is the higher insulin levels that most people have and resulting disease so common today is a result of high insulin levels. But even as AGS is now considered “normal” for those of us longer term KETO/Fasters I can find absolutely no info on the possible ramifications of this higher blood sugar even with low insulin and no insulin resistance issue.
I’m not looking for opinions but links to solid scientific data to explain the AGS and the higher fasting blood sugars longer term and it’s effects.
Thanks

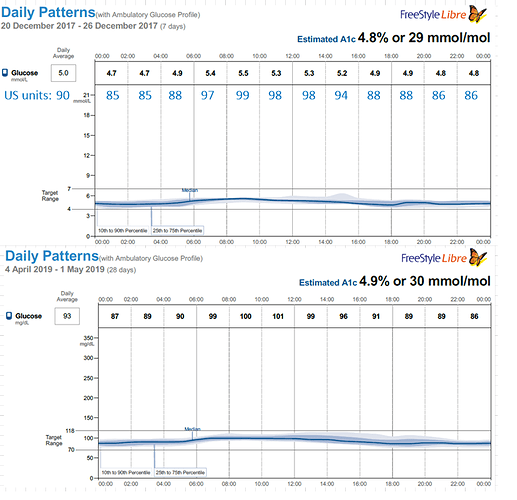
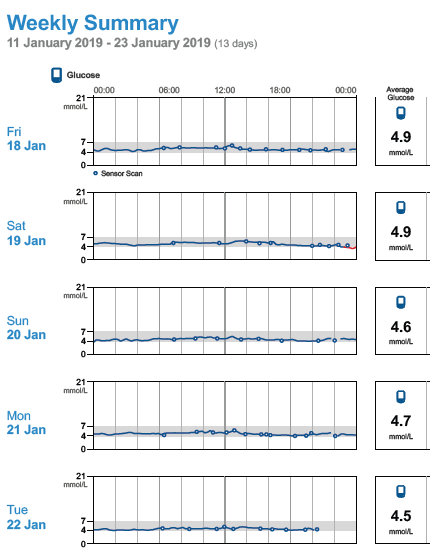
 )
)

 It sure doesn’t surprise me though, that they don’t have the diseases we have. So much of what we eat is just committing slow, suicide:worried:
It sure doesn’t surprise me though, that they don’t have the diseases we have. So much of what we eat is just committing slow, suicide:worried: